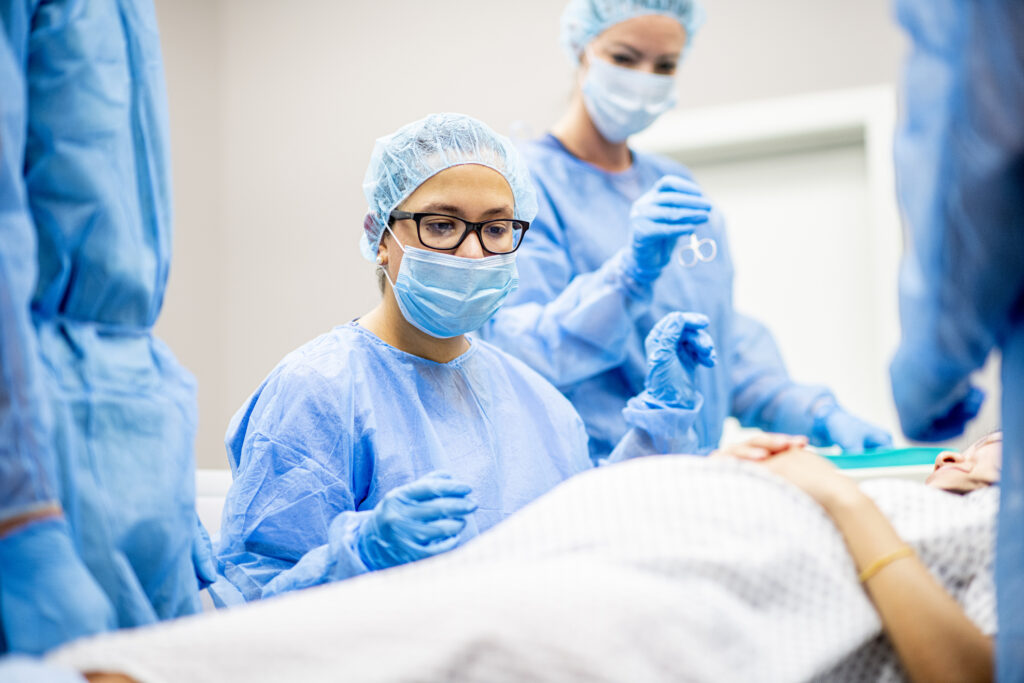
In what’s being called a “first-of-its-kind” procedure, a potentially fatal vascular malformation in an unborn baby was successfully repaired via in-utero brain surgery. Two days after the March 15 operation, the baby girl, named Denver, was successfully delivered and showed progressive normalization of cardiac function, indicating that the most dangerous threats associated with the aggressive vascular malformation, called Vein of Galen malformation, appear to have been avoided.
The results of the study were published May 4 in the peer-reviewed journal Stroke.
The pregnancy was the fourth for Baton Rouge, Louisiana, residents Derek and Kenyatta Coleman, who had not experienced any unusual complications with their first three pregnancies. Genetic testing had furthermore characterized 36-year-old Kenyatta’s pregnancy as “low risk,” according to CNN.
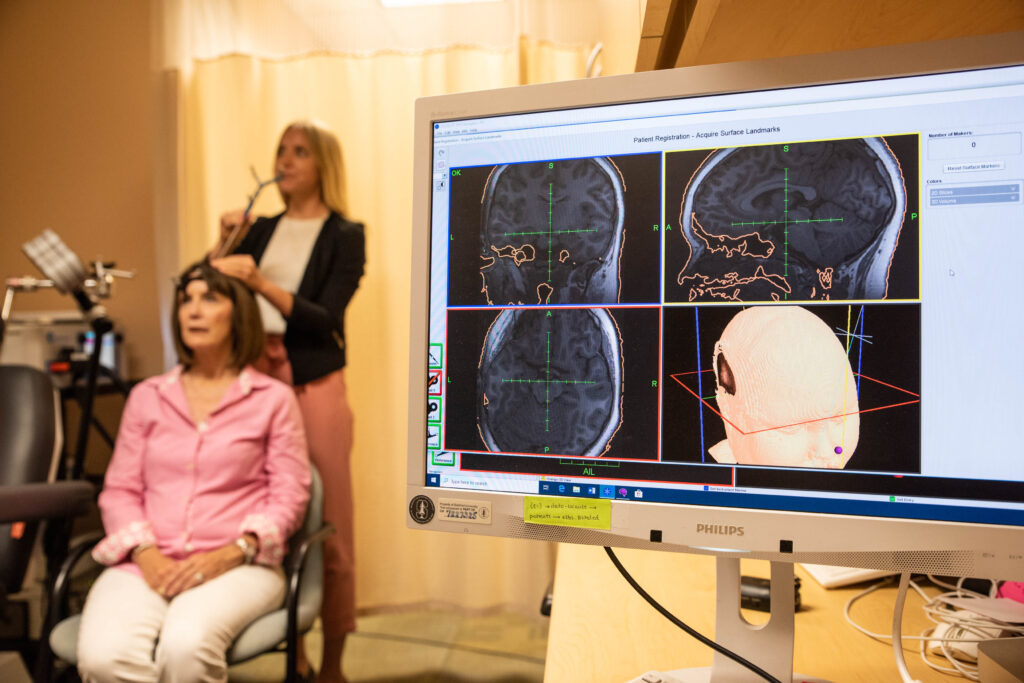
However, at 30 weeks, an ultrasound revealed that there were problems with Denver’s brain and heart, the latter of which was enlarged. Soon after, the infant was diagnosed with VOGM, a rare prenatal condition in which “arteries bringing high-flow, high-pressure blood to the brain from the heart connect directly with one of the main collecting veins deep at the base of the brain, rather than to capillaries that are necessary to slow blood flow and deliver oxygen to surrounding brain tissue. Due to changes in the infant’s vascular physiology during and after the birth process, the high flow in the malformation has an even more serious effect on the heart and brain after birth, putting enormous pressure on the newborn’s heart and lungs,” per a press release from the American Heart Association.
VOGM has a serious impact on newborn heart and lung function, which has been known to cause pulmonary hypertension, heart failure, strokes, fluid buildup, and brain hemorrhage, and other complications.
The disorder is estimated to occur in roughly 1 in every 60,000 births; the current standard of care is post-birth treatment with embolization, a procedure that uses tiny gelatin sponges, beads, or other particles to block a blood vessel. Not only is the procedure risky, it’s not consistently successful at reversing heart failure or mitigating severe brain damage.
The Colemans learned about the clinical trial currently underway at Brigham and Women’s and Boston Children’s hospitals, weighed the risks and the potential for success, and opted to join.
The in-utero brain surgery was performed in the third trimester of pregnancy, when Denver was just 34 weeks and 2 days gestational age. Two days after the procedure, on March 17, Kenyatta gave birth to Denver, who did not require cardiovascular support or additional surgery following the in-utero treatment. She remained in the NICU for several weeks due to prematurity, but during this time showed normal neurological function.
“I heard her cry for the first time and … I can’t even put into words how I felt at that moment,” Kenyatta recalled to CNN, saying it was “the most beautiful moment being able to hold her, gaze up on her, and then hear her cry.”
According to lead study author Dr. Darren B. Orbach, the results are promising. “In our ongoing clinical trial, we are using ultrasound-guided transuterine embolization to address the vein of Galen malformation before birth, and in our first treated case, we were thrilled to see that the aggressive decline usually seen after birth simply did not appear,” said Orbach. “We are pleased to report that at 6 weeks, the infant is progressing remarkably well, on no medications, eating normally, gaining weight, and is back home. There are no signs of any negative effects on the brain.”
Orbach and other medical professionals familiar with both VOGM and embolization caution that this successful surgery is merely the first step in securing more positive outcomes for unborn babies diagnosed with the condition.
RELATED: Man Played His Saxophone While Undergoing Nine-Hour Brain Surgery
“While this is only our first treated patient and it is vital that we continue the trial to assess the safety and efficacy in other patients, this approach has the potential to mark a paradigm shift in managing vein of Galen malformation where we repair the malformation prior to birth and head off the heart failure before it occurs, rather than trying to reverse it after birth,” according to Orbach. “This may markedly reduce the risk of long-term brain damage, disability or death among these infants.”
Pediatric cardiologist Gary M. Satou, who was not involved with the study, concurs that this important milestone must be followed up by additional research and subsequent surgeries on other fetuses diagnosed with VOGM.
“As always, a number of these fetal cases will need to be performed and followed in order to establish a clear pattern of improvement in both neurologic and cardiovascular outcomes,” said Satou. “Thus, the national clinical trial will be crucial in order to achieve adequate data and, hopefully, successful outcomes.”
Said Dr. Colin P. Derdeyn, a neurointerventional radiologist at University of Iowa Health Care who performs VOGM embolizations on newborns and who was not involved with the study: “There are caveats; one successful case is not enough experience for us to conclude that the risks of this procedure are worth the benefits,” later adding: “This is pioneering work being done in a very careful and responsible way.”