A stroke, which takes place when a blood vessel is either blocked by a clot or bursts, depriving the brain of blood, oxygen, and nutrients, can be devastating. According to the American Stroke Association, strokes are the fifth-leading cause of death in the U.S. and a leading cause of disability. Worldwide, the medical emergencies are the second-leading cause of death and the third-leading cause of death and disability combined, based on statistics from the World Stroke Organization.
However, the good news is that roughly 80% of strokes are preventable. Read on for advice about how to recognize the symptoms, what to do if someone is having a stroke, and lifestyle factors that can mitigate your risks.
Common Stroke Symptoms
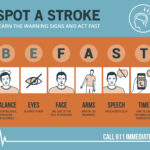
The acronym traditionally used to help people remember stroke symptoms is FAST (face, arms, speech, and time). More recently, medical experts have expanded that to “BE FAST,” with the additions of balance and eyes.
Here’s more on what each letter stands for, and what to look out for, courtesy of First Response Training International:
B — Balance
Nerves that regulate balance and coordination may be affected by a stroke. A sudden inability to walk normally or maintain an upright position are among the more notable symptoms.
E — Eyes
Disruption of normal vision may also be a symptom of a stroke, because lack of blood to the brain can impact the optic nerves. These disruptions to vision do not usually cause pain in the majority of stroke victims. If anything, “the lack of pain should also be interpreted as a symptom and a possible sign of a stroke,” First Response Training International notes.
F — Face
If a person’s face is drooping on one side, particularly when they smile, they may be having a stroke. Asking them to smile will also provide you with an opportunity to assess their mental state and their ability to follow simple instructions, as confusion and/or impaired speech are also stroke symptoms).
A — Arm
A person suddenly becoming unable to raise or hold their arms to shoulder level, assuming they previously were able to do so, may be another indication of stroke. A simple test to see if they can resist opposing force (someone trying to push their arms down from the raised position, for example) can help to assess the situation. If their arms fall or they are unable to hold them up when pressure is applied, they may have suffered a stroke.
S — Speech
Normal speech patterns may be disrupted by stroke. If you’re worried someone could be having a stroke, ask simple questions of the person and look out for any changes in their speech, like slurring or stuttering.
T — Time
Time is critical in the case of a stroke. The American Stroke Association refers to this portion of the acronym as “time to call 911” because stroke victims require immediate medical attention. First Response Training International additionally advises that when you call 911 and communicate your concerns, be sure to note each of the symptoms you have observed and roughly when they started.
Nurse Stephanie Winslow, the stroke coordinator in the Stroke Program at the Baystate Medical Center in Massachusetts, notes that some stroke victims may insist they are fine and express a desire to rest and/or wait and see if the symptoms diminish. Her advice?
“Don’t listen to them and don’t waste time for the symptoms to go away,” Winslow said in a press release. “Stroke is a serious medical emergency and you need to call 911 right away. Never drive the person to the Emergency Department because EMTs can begin life-saving treatment on the way to a designated stroke center like that found at Baystate, which is especially equipped with a stroke team to meet the patient upon arrival at the hospital.”
According to Healthline, additional symptoms not included in the acronym may include confusion, dizziness, and severe headache without a clear cause.
Stroke Risk Factors
Per the American Stroke Association, there are a handful of factors beyond our control that contribute to a higher risk of stroke:
Age: Strokes are more common in those over the age of 65, hence the likelihood of having a stroke increases as we age. That said, it’s important to note that any person of any age can have a stroke, including babies and young children.
Family history: If you have an immediate family member who has had a stroke, particularly before the age of 65, your own risk of having a stroke may be heightened. The risk is also higher if there are certain genetic disorders than run in your family, such as sickle cell anemia, Ehlers-Danlos syndrome, and vasculitis. (Barrow Neurological Institute offers up a more comprehensive list of inherited stroke disorders here.)
Race: Black Americans have higher instances of high blood pressure, diabetes, obesity, sickle cell anemia, and stress, all of which increase the risk of stroke. Black people also have a higher risk of dying from stroke, partly attributed to social determinants of health, such as limited access to medical care, fewer healthy food options, and a lack of green spaces.
Additionally, Hispanics who have limited proficiency in English may not be able to communicate in medical emergencies, which experts suspect has contributed to a higher risk of death from stroke in Latino communities. Per U.S. News and World Report, a projection made by the U.S. Census Bureau anticipates that Hispanic people will comprise nearly 25% of the U.S. population by 2045, while the current nationwide proportion of physicians who identify as Spanish-speaking is less than 6% — highlighting a need for a notable increase in Spanish-speaking medical professionals.
Sex: Females have more strokes than males and are more likely to suffer from fatal strokes. A number of factors can increase the risk of stroke in women, including “pregnancy, history of preeclampsia/eclampsia or gestational diabetes, oral contraceptive use (especially when combined with smoking) and post-menopausal hormone therapy,” the American Stroke Association says.
Medical history: A person who has had a prior stroke, a TIA (transient ischemic attack), or a heart attack is more likely to have a(nother) stroke.
Mental health: Stress and depression are among the mental health issues that can also contribute to heightened stroke risk. According to Healthline, stress increases your risk of high blood pressure, clots, and making unhealthy lifestyle choices. If your mental health is suffering, seek out help and support. Exercise is also important for reducing stress in addition to improving one’s physical health.
Can You Reduce Your Stroke Risk?
Barring factors beyond one’s control, Dr. E. Jesus Duffis, a neurointerventionalist at Baystate Health, has some advice for reducing your risk of having a stroke: don’t smoke (or quit smoking if you do) and see your doctor regularly.
“If you smoke, you’re twice as likely to die if you have a stroke,” Duffis said. “The longer you smoke, the greater the risk. That said, within hours of quitting smoking, your body starts to repair itself. The longer you stay smoke-free, the better your overall health and the lower your risk of stroke.”
Regular checkups are important because they can identify issues like high blood pressure and high cholesterol, potential problems that are often “invisible” or asymptomatic.
“While you can’t control risk factors like age and gender, you can control whether or not you smoke and how well you maintain your health,” continued Duffis. “[They’re] important and powerful first steps to avoiding strokes of all types.”
If you want to learn more about stroke risks and symptoms, check out Stroke.org.
RELATED: It’s World Cancer Day: Prevention Advice From Medical Experts — Exclusive