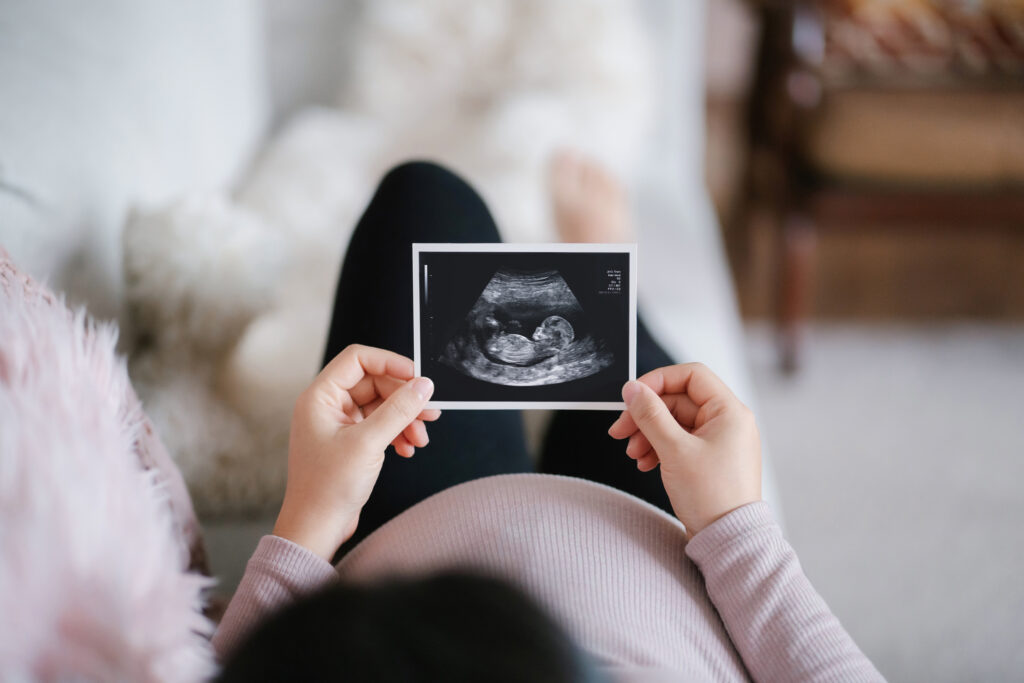
A new study led by doctors at St. George’s, University of London has shown that scheduling a third trimester scan during pregnancy can greatly reduce the number of unexpected breech births as well as reduce the risk of severe health complications in newborns.
The findings, published in PLOS Medicine in April, determined that the additional, late-term scan could lower the number of unexpected breech births by up to 70%, as the baby’s position at that point will help indicate the position at the time of birth.
A breech birth is one in which the baby has turned in the womb and is positioned feet or bottom first. It can cause a lack of oxygen that can lead to an increased risk of a brain injury and other conditions requiring neonatal unit care. Such a position could even result in the death of the baby.
According to the study, the rate of incidence of babies in breech at term falls between 3% and 4%. Vaginal breech delivery is correlated with an increase in perinatal or neonatal mortality and morbidity, meaning death or injury to the baby, and maternal morbidity. Correct knowledge of the baby’s position at a pregnancy’s term is “essential” for providing adequate maternity care and the opportunity for women to be counseled about their options, including vaginal birth or cesarean birth. The study notes that clinical exams are “not accurate enough” to gather such information when compared to ultrasound scans.
Currently, it’s routine for pregnant women to get scans around weeks 12 and 20, but the study authors suggest standardizing another at weeks 36 or 37. Third trimester scans are not common, and generally only take place if there is a risk of pregnancy complications, like high blood pressure or diabetes, that require further observation.
“It’s vital we know how the baby is lying towards the end of pregnancy as we want to avoid a breech birth if at all possible,” lead author Asma Khalil said in a press release. “The two routine scans are far too early to tell us how the baby will be positioned at the time of labor and that’s why a third scan at 36-37 weeks could be a game-changer to pregnancy and birth care.”
RELATED: Diverse Nurse Workforce Linked to Improved Maternal Health Outcomes: Study
The study tracked pregnant patients at St. George’s University Hospital NHS Foundation Trust and Norfolk and Norwich University Hospital NHS Foundation Trust, with doctors comparing the rate of unexpected breech births and infant health after third trimester scan policies were implemented there.
At the St. George’s location, 24,128 pregnant women were included in the study, with 16,777 receiving only the usual 12 and 20-week scans, and 7,351 receiving an additional ultrasound at 36 weeks from a sonographer. At the Norfolk and Norwich location, 9,694 women participated, with 5,119 receiving the standard 12 and 20-week scans, and 4,575 being given a “point-of-care” ultrasound scan at 36 weeks with an inexpensive hand-held device, which midwives can be trained to use.
Both types of third trimester scans resulted in a radical reduction of unexpected breech births: St. George’s patients experienced a 71% lower rate, and Norfolk and Norwich patients a 69% lower rate.
Fran Harlow, a consultant obstetrician for the Norfolk and Norwich University Hospital, said the findings are extremely encouraging.
“We are delighted that this study has shown that the benefits to the mother and baby are equivalent to a formal scan performed by an ultrasonographer,” she said in a statement. “This keeps care in the community and [women] centered. We hope that the data from NNUH and St. George’s provides the stimulus for a national policy of third trimester scanning. In addition, this study has demonstrated that use of a hand-held ultrasound device by a midwife is an innovative, progressive, and now proven, way of achieving this.”
If you’d like to support moms and babies around the world, consider donating to Nice News’ latest fundraiser, benefitting Every Mother Counts in honor of Mother’s Day in May.